PTSD Symptoms are critical to recognize early, as post-traumatic stress disorder (PTSD) can develop after a person experiences or witnesses a traumatic event. Recognizing PTSD symptoms early makes effective treatment more likely. This guide explains common PTSD symptoms, how clinicians assess and diagnose the condition, and evidence-based treatment options. Many people with PTSD feel isolated or overwhelmed; identifying PTSD symptoms and reaching out for care can lead to meaningful recovery and improved daily functioning. We also summarize diagnostic criteria and practical treatment approaches, including psychotherapy and medication management, to give a straightforward, usable overview.
PTSD Symptoms, Recognition, Diagnosis, and Treatment Guide
PTSD symptoms can cause difficulties that interfere with work, relationships, and overall wellbeing. Spotting these PTSD symptoms is the first step toward getting help. Symptoms generally fall into four groups: intrusive memories, avoidance, negative changes in mood and thinking, and altered arousal or reactivity. Organising PTSD symptoms this way helps guide assessment and timely treatment planning.
Understanding PTSD Symptoms:
PTSD symptoms arise after exposure to a traumatic event and can affect people of any age or background. It often involves intense fear, helplessness, or horror and can lead to long-lasting psychological distress that disrupts daily life. Understanding common triggers and effects helps patients and families recognise when professional support is needed.
Common PTSD Symptoms:
PTSD symptoms can produce disruptions in everyday life. Early recognition supports faster access to care. Common PTSD symptoms include:
- Flashbacks: Reliving the traumatic event as though it is happening again.
- Nightmares: Distressing dreams connected to the trauma.
- Avoidance behaviors: Deliberately avoiding people, places, conversations, or situations that remind you of the trauma.
- Negative mood changes: Persistent feelings of hopelessness, detachment, guilt, or emotional numbness.
How to Recognize Intrusive Memories and Flashbacks in PTSD Symptoms
Intrusive memories and flashbacks are central PTSD symptoms. They often arrive suddenly and can be triggered by sounds, smells, images, or other sensory cues tied to the event. Flashbacks can feel vivid and overwhelming, as if the trauma is happening again. Practical coping tools — such as grounding exercises and brief mindfulness practices — can reduce distress and help someone return to the present moment.
What Are Avoidance Behaviors and Negative Mood Symptoms in PTSD?
Avoidance strategies are attempts to reduce distress by steering clear of reminders of the trauma. That may include avoiding conversations, locations, or people connected to the event. Negative mood changes commonly include persistent sadness, anger, guilt, or a sense of emotional numbness. These PTSD symptoms affect relationships and daily functioning and should be addressed in treatment planning.
Recognition and Diagnosis of PTSD Symptoms:
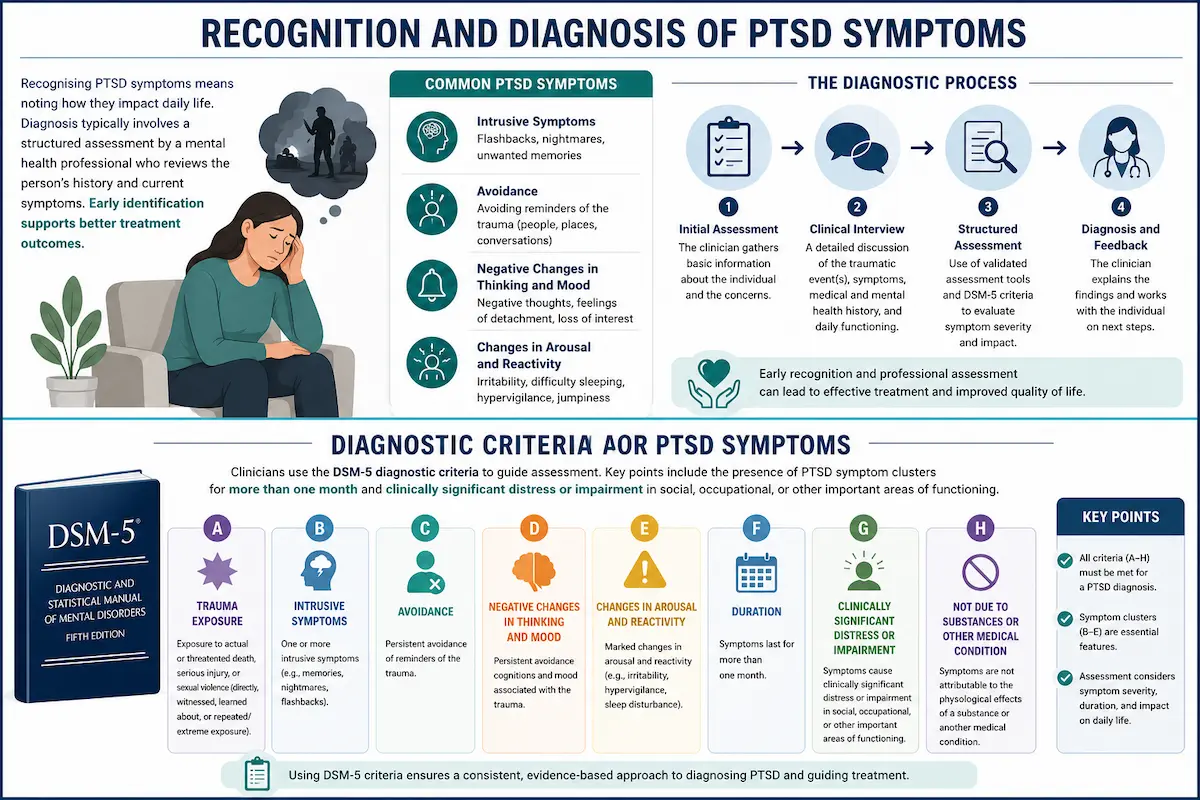
Recognising PTSD symptoms means noting how they impact daily life. Diagnosis typically involves a structured assessment by a mental health professional who reviews the person’s history and current symptoms. Early identification supports better treatment outcomes.
Diagnostic Criteria for PTSD Symptoms:
Clinicians use the DSM-5 diagnostic criteria to guide assessment. Key points include the presence of PTSD symptom clusters for more than one month and clinically significant distress or impairment in social, occupational, or other important areas of functioning.
What Are the DSM-5 Criteria for PTSD Symptoms Diagnosis?
The DSM-5 requires exposure to a qualifying traumatic event plus symptoms from the core clusters: intrusive symptoms, avoidance, negative alterations in mood and cognition, and increased arousal/reactivity. Familiarity with these PTSD symptom criteria helps patients and clinicians decide whether further evaluation is needed.
| DSM-5 PTSD Symptom Clusters | Description |
|---|---|
| Intrusive Symptoms | Recurrent, involuntary, and distressing memories, flashbacks, or nightmares related to the trauma. |
| Avoidance | Efforts to avoid distressing memories, thoughts, feelings, or external reminders of the traumatic event. |
| Negative Alterations in Mood and Cognition | Persistent negative beliefs, distorted blame, reduced interest in activities, feelings of detachment, or difficulty experiencing positive emotions. |
| Increased Arousal and Reactivity | Irritability, hypervigilance, an exaggerated startle response, concentration problems, or sleep disturbances. |
How Does a Psychiatric Evaluation Assess PTSD Symptoms?
A psychiatric evaluation uses a detailed clinical interview, a review of medical and trauma history, and often standardized assessment tools to document PTSD symptoms and functioning. Clinicians assess co-occurring conditions and safety concerns and then create a personalised treatment plan based on the individual’s needs and goals.
Treatment Approaches for PTSD Symptoms:
Effective PTSD care commonly combines psychotherapy, medication management, and lifestyle supports. Knowing these options helps patients choose treatments that fit their goals and circumstances.
Trauma-Focused Psychotherapy for PTSD Symptoms:
Trauma-focused psychotherapy is a first-line treatment for PTSD symptoms. These therapies help patients process traumatic memories and reduce symptoms. Common evidence-based approaches include cognitive behavioral therapy (CBT) and eye movement desensitization and reprocessing (EMDR), both backed by research for treating trauma-related symptoms.
Medication Management for PTSD Symptoms:
Medication can be a helpful component of PTSD symptoms treatment. Antidepressants, particularly selective serotonin reuptake inhibitors (SSRIs), are frequently used to reduce symptoms and stabilise mood. Regular monitoring and follow-up ensure medications are working and side effects are managed.
Mindfulness and Grounding Techniques for PTSD Symptoms:
Mindfulness and grounding exercises support PTSD symptom management by encouraging present-moment awareness and reducing physiological arousal. Techniques such as paced breathing, brief meditations, and sensory grounding can be used in conjunction with formal therapies.
Lifestyle Recommendations to Support PTSD Symptoms Recovery:
Healthy daily habits support recovery from PTSD symptoms. Regular physical activity, balanced nutrition, good sleep hygiene, and a dependable support network can strengthen resilience and improve everyday functioning. These steps complement clinical treatment.
Telepsychiatry for PTSD Symptoms Treatment:
Telepsychiatry expands access to psychiatric care by offering remote appointments. It can be especially helpful for people living in rural or underserved areas and improves continuity of care and scheduling flexibility.
Our Approach to PTSD Symptoms Care:
At Resilience Psychiatry, we follow a trauma-informed approach and design personalised treatment plans tailored to each patient’s history and goals. Our multidisciplinary team provides comprehensive evaluations, medication management, and evidence-based therapies to support recovery and long-term wellbeing.
What Are the Common PTSD Symptoms and Signs of Post Traumatic Stress Disorder?
Common PTSD symptoms include emotional signs (anxiety, depression), cognitive signs (intrusive thoughts, memory difficulties), and physical signs (hypervigilance, sleep problems). Symptom patterns vary between individuals, so assessments should be tailored to each person.
How Is PTSD Diagnosed? Understanding the Diagnostic Criteria and Evaluation Process for PTSD Symptoms
PTSD diagnosis involves a structured clinical evaluation that documents symptoms, duration, and functional impact. Clinicians apply DSM-5 criteria and use validated assessment tools to ensure an accurate diagnosis and to guide treatment planning.
Research also shows how diagnostic criteria have evolved and what that means for assessing trauma exposure and PTSD symptoms.
PTSD Diagnosis: DSM-5 Criteria & Assessment
The DSM-5 introduced important revisions to the diagnostic criteria for posttraumatic stress disorder, which required corresponding updates to assessment measures. This work outlines the specific changes to the criteria and to National Center for PTSD assessment tools, and it discusses how the revised criteria affect evaluation of trauma exposure and PTSD symptoms. While the DSM-5 definition differs from earlier editions in some respects, the authors note continuity with the original DSM-III view of PTSD as a chronic, potentially debilitating disorder following catastrophic life events.
Posttraumatic stress disorder in DSM-5: New criteria, new measures, and implications for assessment, FW Weathers, 2014
What Treatment Options Are Available for PTSD Symptoms? Psychotherapy, Medication, and Telepsychiatry Explained
Several effective treatment options exist for PTSD symptoms, including trauma-focused psychotherapy, medication management, and telepsychiatry. Treatments can be combined and adapted to meet each patient’s needs for better outcomes.
How Does Cognitive Behavioral Therapy and EMDR Help Treat PTSD Symptoms?
Cognitive behavioral therapy (CBT) and eye movement desensitization and reprocessing (EMDR) are evidence-based treatments for PTSD symptoms. CBT targets unhelpful thoughts and behaviors, helping people build coping skills, while EMDR supports processing of traumatic memories using guided bilateral stimulation.
Clinical studies support the effectiveness of trauma-focused psychotherapies, including CBT and EMDR, in reducing PTSD symptoms.
Effectiveness of Trauma-Focused Psychotherapy for PTSD Symptoms
ABSTRACT: This retrospective evaluation compared trauma-focused psychotherapy (TF-P) with stabilization-and-waiting among patients diagnosed with complex post-traumatic stress disorder (CPTSD) using ICD-11 criteria. The study identified patients treated at a specialist trauma service over three years through self-report measures, file review, and clinician opinion. Patients received a phase-based program: phase 1 emphasized stabilization and safety, followed by a waiting period; phase 2 delivered individual TF-P such as TF-CBT, EMDR, or a combination. The primary outcome compared PTSD symptoms during phase 2 versus phase 1; secondary outcomes included depressive symptoms, functional impairment, and a proxy measure of CPTSD.
The effectiveness of trauma-focused psychotherapy for complex post-traumatic stress disorder: A retrospective study, E Melegkovits, 2023
What Role Do Medication Management and SSRIs Play in PTSD Care?
Medication management, particularly with SSRIs, is an important part of care for many patients with PTSD symptoms. These medications can stabilise mood and reduce anxiety, making it easier to engage in therapy and daily activities.
Clinical research consistently supports SSRIs as a well-established first-line pharmacotherapy for PTSD symptoms.
Pharmacotherapy for PTSD Symptoms: SSRIs as First-Line Treatment
Post-traumatic stress disorder affects roughly 7.8% of people over a lifetime and is associated with functional impairment, suicidal behaviour, and frequent comorbidity. Research shows PTSD responds to both pharmacotherapy and psychotherapy. Selective serotonin reuptake inhibitors (SSRIs) are the most extensively studied medications for PTSD symptoms, with sertraline, paroxetine, and fluoxetine receiving substantial research attention; sertraline and paroxetine are US FDA-approved for PTSD. Short-term trials (6–12 weeks) demonstrate efficacy, and continuation or maintenance treatment for 6–12 months reduces relapse risk. SSRIs generally have a favourable adverse-effect profile, supporting their role as first-line agents; non-SSRI options are considered when SSRIs are not tolerated or are ineffective.
SSRIs versus non-SSRIs in post-traumatic stress disorder: an update with recommendations, 2004
| Common SSRIs Used in PTSD Treatment | Key Information |
|---|---|
| Sertraline | FDA-approved for PTSD; effective in reducing symptoms and generally well-tolerated. |
| Paroxetine | FDA-approved for PTSD; can help with anxiety and mood stabilization; requires monitoring for side effects. |
| Fluoxetine | Widely studied; not FDA-approved specifically for PTSD but commonly prescribed and effective for symptom management. |
How Can Telepsychiatry Enhance Access to PTSD Symptoms Treatment?
Telepsychiatry improves access by offering remote consultations with mental health professionals. It reduces geographic and mobility barriers and helps patients maintain continuity of care.
What Are the Benefits of Telepsychiatry Services for PTSD Patients?
Telepsychiatry increases convenience, protects privacy, and broadens access to specialists. Patients can attend sessions from home, lowering common barriers to care and supporting consistent treatment.
How to Schedule and Prepare for a Telepsychiatry Appointment for PTSD Symptoms?
To book a telepsychiatry visit, contact your provider or use the clinic’s scheduling system. Prepare by finding a quiet, private space and making sure your device and internet connection are ready for the session.
What Coping Strategies and Support Resources Are Effective for Managing PTSD Symptoms?
Effective coping and support combine professional treatments, structured self-help techniques, and crisis resources. Using these options alongside clinical care improves PTSD management and builds resilience.
Which Self-Help Techniques Support PTSD Relief?
Self-help strategies such as mindfulness, journaling, and creative activities can reduce distress and improve emotional regulation. These techniques complement therapy and can be tailored to personal preferences.
When Should You Seek Professional Help for PTSD?
Seek professional help when PTSD cause ongoing distress, interfere with daily life, or include thoughts of self-harm. A mental health professional can assess risk, recommend treatment, and coordinate care. If you are ready to seek help, contact us to learn more about our services.
Frequently Asked Questions:
What are the long-term effects of untreated PTSD?
Untreated PTSD can lead to long-term problems, including chronic anxiety and depression, substance misuse, and strained relationships. It can also affect physical health, contributing to conditions like cardiovascular disease and chronic pain through prolonged stress. Early intervention lowers these risks and supports recovery.
How can family and friends support someone with PTSD?
Family and friends can help by listening without judgment, being patient, and encouraging professional care. Creating a safe, understanding environment helps the person feel accepted. Learning about PTSD symptoms equips loved ones to offer practical, informed support.
Are there specific lifestyle changes that can help manage PTSD?
Several lifestyle changes can reduce PTSD. Regular physical activity (walking, yoga, swimming), a nutritious diet, and consistent sleep routines support emotional regulation. Building social connections and participating in community or leisure activities can reduce isolation and boost resilience.
What role does mindfulness play in PTSD treatment?
Mindfulness helps people stay present and observe thoughts and feelings without judgment. Practices like meditation and controlled breathing can reduce anxiety and help manage intrusive memories. Mindfulness often complements trauma-focused therapies and can improve overall treatment outcomes.
How can someone find a qualified mental health professional for PTSD?
To find a qualified provider, ask for referrals from your primary care doctor or trusted contacts, use professional directories, and check credentials and trauma specialization. Consider the clinician’s experience, treatment approaches, and whether they provide trauma-informed care. Feeling safe and understood by your provider is essential to effective treatment.
What are the differences between PTSD and Complex PTSD?
PTSD often follow a single traumatic event, while Complex PTSD arises from prolonged or repeated trauma, such as ongoing abuse or neglect. Complex PTSD can include additional challenges like difficulties with emotional regulation, a negative self-concept, and persistent relationship problems. Distinguishing the two helps guide diagnosis and the need for specialised, phase-based treatment approaches.